Alternate Day Iron Dosing: Does It Work?
The claim is that we can biohack our way against the rise in hepcidin by skipping a day between iron doses. Here we take a look at the data.
After releasing my Iron Deficiency Protocol, several people asked me about alternate-day dosing.
Here’s the hypothesis: when you take iron, it spikes the hormone hepcidin; hepcidin shuts down iron absorption; therefore, if you wait till hepcidin goes back down, the next dose will have higher bioavailability. Higher bioavailability over time leads to better cumulative iron absorption.
My critique: as covered in Understanding Iron, the reason hepcidin responds to iron status is to ensure optimal iron status with as little influence of your diet as possible; if iron status goes up over a few weeks, all this does is generate even more hepcidin; therefore, all things related to properly functioning hepcidin should mean revert over time, meaning they just go back to the way they were.
This is educational in nature and not medical or dietetic advice. See terms for additional and more complete disclaimers.
Since we know that iron status going up makes the absorption of iron from food and supplements go down, to show something novel and practical these studies have to show that you can get the total amount of iron absorbed per unit time higher by introducing a complication into the dosing schedule.
In other words, it is obvious that if you allow for a longer time, you can get more iron absorbed, and it is obvious that if you consume less iron, you will absorb more from food and supplements. What is not so obvious is whether taking iron every other day instead of taking it every day can give you greater total iron absorption over the course of a particular unit of time, such as a month, or six months.
The first of these studies was Stoffel, 2017. The dosing schedule was 60 milligrams of iron from ferrous sulfate either every day for 14 days, or every other day for 28 days.
The fractional iron absorption increased from 16.3% to 21.8% on the alternate day dosing, a relative increase of 33.7%. The total iron absorption increased from 131 milligrams to 175.3 milligrams, a relative increase of 33.8%.
However, the alternate dosing group was given twice the amount of time to absorb the iron!
That means the absorption of iron per unit time FELL from 65.5 milligrams per week to 43.8 milligrams per week, a relative LOSS of 33%.
The study presents the data in a way that makes the regimen look 34% better when it is actually 33% worse.
Oflas, 2020 then compared 160 milligrams per day to 80 milligrams per day to 80 milligrams every other day for one month. Hemoglobin rose similarly in all three groups, ferritin rose the most in the first group, and side effects were highest in the first group and lowest in the third group. They didn’t measure iron absorption. All this shows is that 40 milligrams per day is plenty and 160 milligrams per day is too much.
Mehta, 2020 then compared 60 milligrams every day to 60 milligrams every other day for 21 days. Nausea and metallic taste drove higher total side effects in the every day group, while hemoglobin increased more in the alternate day group. This implies that 30 milligrams per day works better than 60 milligrams per day. This contrasts with Oflas, 2020, where the hemoglobin rise was similar across groups, although Oflas made 40 milligrams per day look sufficient, which is close to 30 milligrams per day. This study did not look at total iron absorbed. Hemoglobin was the only variable they reported at 21 days, which makes them look like they were cherry-picking their data.
A meta-analysis published this year ranked this study as the one out of five randomized trials that had a high risk of bias, due to unclear description of the randomization process, deviation from the original protocol, and selective reporting of results.
Kaundal, 2020 compared 60 milligrams twice a day for three weeks to 120 milligrams taken every other day for six weeks. They received the same total amount of iron, but as with Stoffel, 2017, the alternate-day group was given twice as much time to absorb the iron. Despite this, the hemoglobin response was better in the twice a day group, and side effects were greater too. This study did not measure iron absorption.
Stoffel, 2020 looked at alternate versus daily dosing of an iron-fortified porridge and alternate versus every-third-day dosing of an iron supplement in Kenyan babies, with 12 milligrams of iron in each dose, focusing on changes occurring within four days of the regimen. There was no difference in fractional iron absorption after the second porridge meal between the consecutive and alternate-day regimens, nor after the second dose of the two supplement regimens. This obviously suggests that daily dosing would provide more absorbed iron than alternate or every-third-day dosing.
Kaynar, 2022 compared 160 milligrams every day to 160 milligrams every other day over the course of 60 days. At the end of the study, the values for hemoglobin, ferritin, transferrin saturation, and everything else were practically identical. They did not report iron absorption or side effects. This suggests 80 milligrams of iron per day is plenty and that 160 milligrams per day is a waste, which is consistent with Oflas, 2020’s suggestion that 40 milligrams per day is plenty.
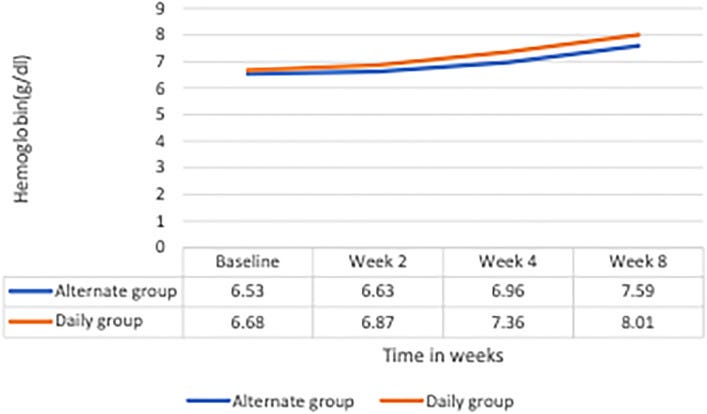
Pasupathy, 2023 compared 120 milligrams every other day to 60 milligrams per day for two months. They placebo-controlled the treatment by having everyone take two tablets per day and spacing the placebo and iron tablets differently in the two groups. This is the first of these studies to equate both the total dose of iron taken and the total time over which it was taken.
The rise in hemoglobin was not statistically different between groups, though it appears slightly better in the daily group and the gap widens over time, suggesting the daily group might prove superior if given months instead of weeks:
At week 4, there was five times as much nausea in the alternate day group than in the daily group, but by week 8 this evened out and there were no other differences between groups in adverse effects.
Stoffel, 2023 then really pushed the boundaries of an absolutely bizarre study design. One group got 100 milligrams of iron every day for 90 days and then a placebo for 90 days. The other group got 100 milligrams of iron one day alternated with a placebo the next day, repeating for 180 days. At the 93-day mark, hemoglobin, ferritin, and transferrin saturation were all higher in the daily group. At the 186-day mark, hemoglobin levels were identical between the two groups. Hematocrit was identical. Transferrin saturation and ferritin were better in the alternate-day group. Side effects were higher in the daily group than in the alternate-day group throughout the study.
Now, at this point Stoffel finally joined the ranks of Pasupathy in equating for both cumulative iron intake and time. However, that span of time involved 3 months straight of taking a placebo for one group. This, then, completely left the realm of any practical utility. Who on earth would adopt a regimen of alternating quarterly between supplementing and not supplementing iron daily?
A systematic review published this May, covering everything except Stoffel, 2023, concluded that alternate-dosing has no impact on hemoglobin or iron markers but reduces the risk of side effects.
But every single one of these studies used ferrous sulfate, famous for its gastrointestinal side effects!
There are other ways to avoid these side effects. Focus on food, or on a different type of iron supplement.
Further, none of these studies support doses higher than 40 milligrams per day doing anything better than 30-40 milligrams per day, and those that do compare dosing almost universally show that 30-40 milligrams per day greatly reduces side effects compared to higher doses.
The only two studies that controlled for the total amount of iron given per unit time were Pasupathy, 2023 and Stoffel, 2023:
Stoffel, 2023 simply showed that taking iron every day can normalize hemoglobin 3 months faster than taking it every other day, and that if you go three months without taking any iron after three months of taking 100 milligrams per day your iron markers will drop.
Pasupathy, 2023 is the only study to control for total iron per unit time and to do so in a realistic regimen: take half as much every day perpetually, or take twice as much every other day perpetually. It suggested that overall there is no difference in anything when using an average dose of 60 milligrams per day, but it hinted that over a period much longer than 8 weeks, the daily dose might prove superior in raising hemoglobin.
Thus, in this growing body of literature there is really no indication of anything other than that 30-40 milligrams of iron per day is safer than taking much larger doses, that much larger doses have no additional utility, and that alternate dosing schemes introduce extra complications with no benefit.
For this reason, alternate-dosing iron supplementation is not included in my Iron Deficiency Protocol.


This article was really helpful. Had been wondering about this!
Is there data on whether heme iron, either supplement or from food, creates a different hepcedin response than elemental iron like ferrous sulfate or an iron amino acid chelate?